A new report from the LeadingAge LTSS Center @UMass Boston and Collective Insight shares the experiences of residents, family caregivers, and nurses in Massachusetts assisted living residences (ALRs) during the pandemic, when an executive order allowed ALR nurses to deliver certain basic health services such as giving injections, dressing simple wounds, and applying ointments and drops. The benefits of this change cited in the report, “Provision of Skilled Nursing Care by Assisted Living Residences: Stakeholder Views on the COVID-19 Experience,” include perceived improvements in the coordination and timeliness of care along with reduced financial and emotional burdens for residents and their families by delaying the need to move to a nursing facility.
For years, Massachusetts law has stipulated that ALR nurses cannot provide basic health services. Instead, residents and their families have needed to either provide that care themselves, hire skilled nurses to come to their residence, or move the resident to a nursing home — where daily costs are much higher, but paid for by Medicaid when personal funds are depleted. As with many challenges related to long-term supports and services, the COVID-19 pandemic shone a spotlight on this restriction. At the height of the pandemic, bringing outside family members or nurses into ALRs put those nurses, the residents and their families, and other staff at risk. In April 2020 Governor Charlie Baker issued an executive order that allowed residents the option to receive this care from ALR nurses.
To understand the impact of this change, Massachusetts Assisted Living Association (MASS-ALA) engaged researchers Erin McGaffigan, PhD, principal of Collective Insight and a research fellow at the LeadingAge LTSS Center @UMass Boston, and Marc Cohen, PhD, clinical professor of gerontology at UMass Boston and co-director of the LeadingAge LTSS Center @UMass Boston and research director at Community Catalyst.
The authors took time early in the research design process to hear directly from stakeholders to determine focus areas for their interviews, which included investigating nurse training needs and residents’ quality of life. Stakeholder engagement in research design is not new for McGaffigan and Cohen, who also co-lead an engaged research grant funded by the Patient-Centered Outcomes Research to train gerontologists on engaged research. “Taking the time up front to understand the research context and the most feasible ways to collect data makes data collection possible and data more useful, even during times of pandemic worker shortages,” says McGaffigan.
“Qualitative research does not seek to answer yes or no to a particular question,” McGaffigan says. Instead, “We explore the stories, and in doing so, highlight the unexpected impact of policy change and the key elements for consideration if the change becomes permanent. Overall, I was most surprised by the impact this policy had on residents with diabetes, who up until this executive order could only live in ALRs if they could provide the care on their own or hire assistance.”
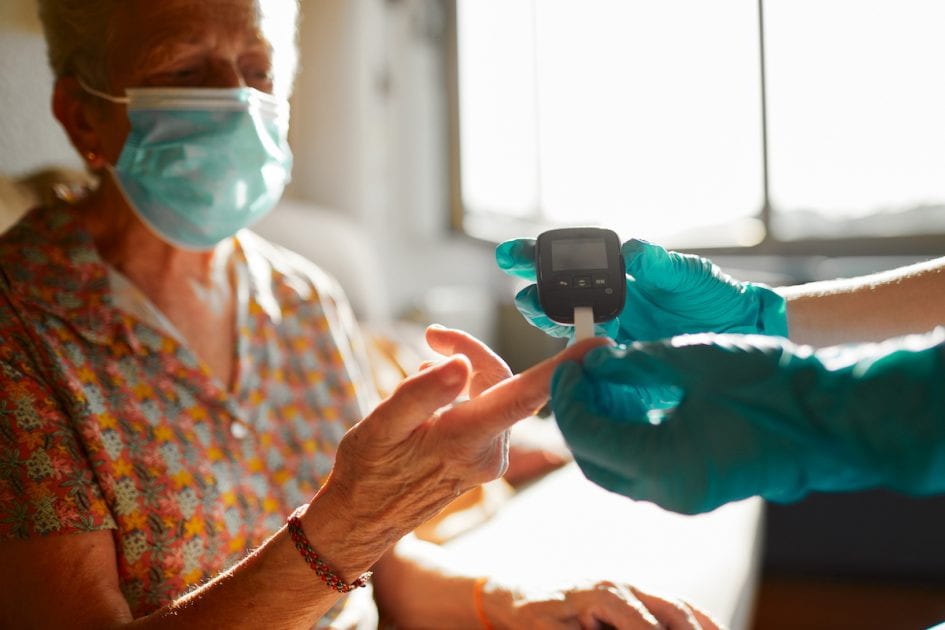
A key finding of the ALR study was that residents with insulin-dependent diabetes and their families found the new nursing provision to be a “life changer.” Allowing ALR staff nurses to monitor blood sugar and give insulin injections saved costs for the families while ensuring more consistent care since the ALR nurses were familiar with residents’ needs, provided insulin before meals, and monitored diabetic symptoms throughout the day. Other findings: Basic skilled care by ALR nurses did not replace the need for skilled care agencies to provide residents with more elaborate wound care, for example. Most interviewees wanted ALRs to retain their social, community feel even if ALR nurses provide additional basic health services. The nurses interviewed also pointed to the need for additional refresher training before providing basic care.
Efforts are underway to make the skilled nursing change permanent. In February 2022, Governor Baker signed a broad spending bill that includes extending the allowance until July 15 or the end of the public health emergency, whichever comes first. Senate Bill 409, which would make the provision permanent, was favorably voted out of the Joint Committee on Elder Affairs in the Massachusetts Legislature and is awaiting Baker’s signature.
“Now more than ever, we need a permanent solution to ensure that older adults have access to the same basic assisted living services that are available in most states, including New Hampshire, Rhode Island, Connecticut, and New York,” says Brian Doherty, president and CEO of MASS-ALA.

Leave a Reply