In today’s health-conscious world, weight loss surgery has emerged as a viable solution for individuals struggling with obesity or metabolic disorders. While lifestyle changes like diet and exercise remain foundational, bariatric procedures offer medically supervised, sustainable weight loss for those who qualify. Understanding the 5 weight loss surgery options available can help patients make informed decisions tailored to their health needs.
Understanding the Need for Weight Loss Surgery
Obesity affects millions worldwide, increasing the risk of:
-
Type 2 diabetes
-
Hypertension and cardiovascular disease
-
Sleep apnea
-
Joint problems
Conventional weight loss strategies may be insufficient for individuals with severe obesity (BMI ≥ 40) or those with obesity-related comorbidities. Bariatric surgery not only promotes weight reduction but also improves metabolic function, often leading to the remission of diabetes and enhanced quality of life.
The Science Behind Bariatric Surgery
All 5 weight loss surgery options share common mechanisms to aid weight reduction:
-
Restriction: Limiting stomach capacity reduces food intake (e.g., sleeve gastrectomy).
-
Malabsorption: Altering the digestive tract reduces calorie and nutrient absorption (e.g., biliopancreatic diversion).
-
Hormonal Regulation: Surgery can modify gut hormones like ghrelin, leptin, and GLP-1, which control appetite, satiety, and glucose metabolism.
-
Behavioral Reset: Postoperative dietary guidance reinforces mindful eating habits and lifestyle changes.
These physiological effects work synergistically to support long-term fat loss, improve insulin sensitivity, and reduce obesity-related complications.
Overview of 5 Weight Loss Surgery Options
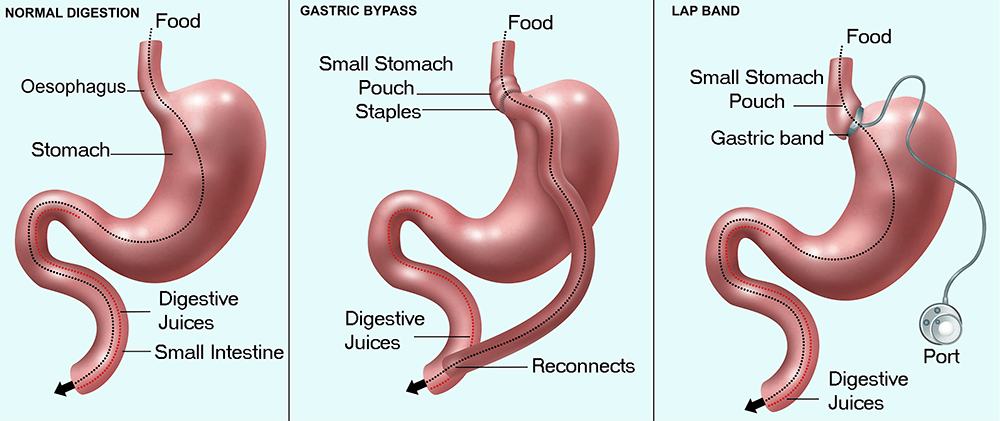
1. Gastric Bypass (Roux-en-Y)
Mechanism: Combines restriction and malabsorption by creating a small stomach pouch and rerouting the small intestine.
Benefits:
-
Significant and rapid weight loss (average 60–70% excess weight loss in 1–2 years)
-
Improves type 2 diabetes and lipid profiles
-
Hormonal changes reduce appetite
Considerations:
-
Higher risk of nutrient deficiencies (iron, B12, calcium)
-
Requires lifelong supplementation
Candidate Profile: Individuals with BMI ≥ 40 or BMI ≥ 35 with comorbidities.
2. Sleeve Gastrectomy
Mechanism: Removes approximately 80% of the stomach, creating a tubular “sleeve.”
Benefits:
-
Restrictive effect reduces food intake
-
Hormonal modulation reduces ghrelin (hunger hormone)
-
Lower complication risk than gastric bypass
Considerations:
-
Irreversible
-
Potential for acid reflux or gastric sleeve leaks
Candidate Profile: Patients seeking a simpler surgical procedure with lower risk but still significant weight loss.
3. Adjustable Gastric Band (Lap-Band)
Mechanism: A silicone band is placed around the upper stomach, adjustable to restrict food intake.
Benefits:
-
Reversible and adjustable
-
Gradual weight loss
-
Minimally invasive with shorter hospital stay
Considerations:
-
Slower weight loss compared to other surgeries
-
Risk of band slippage or erosion
-
Requires frequent follow-up for band adjustments
Candidate Profile: Patients preferring a reversible procedure and committed to long-term follow-up.
4. Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
Mechanism: Combines sleeve gastrectomy with significant intestinal bypass to reduce calorie absorption.
Benefits:
-
Maximum weight loss potential (70–80% excess weight loss)
-
Highly effective for resolving diabetes
-
Alters gut hormones to improve satiety
Considerations:
-
Higher risk of malnutrition and vitamin deficiencies
-
More complex surgery with longer recovery
Candidate Profile: Severe obesity (BMI ≥ 50) or individuals needing maximal weight reduction.
5. Endoscopic Sleeve Gastroplasty (ESG)
Mechanism: Minimally invasive procedure using endoscopic sutures to reduce stomach volume without incisions.
Benefits:
-
Non-surgical, no external scars
-
Moderate weight loss (approx. 15–20% total body weight in 1 year)
-
Lower complication rate
Considerations:
-
Less weight loss than traditional bariatric surgery
-
Requires strict dietary adherence post-procedure
Candidate Profile: Patients preferring a minimally invasive, reversible option or those not eligible for major surgery.
Research and Evidence Supporting Weight Loss Surgeries
-
Gastric Bypass & Sleeve Gastrectomy: Human studies show 50–70% excess weight loss within 1–2 years and remission of type 2 diabetes in 60–80% of patients.
-
BPD/DS: Clinical trials indicate highest long-term weight loss but increased risk of nutrient deficiencies.
-
Adjustable Gastric Band: Meta-analyses report 40–50% excess weight loss with long-term follow-up needed for band adjustments.
-
Endoscopic Sleeve Gastroplasty: Emerging evidence demonstrates 15–20% total body weight loss at 12 months with low complication rates.
Practical Guidelines Post-Surgery
Although these surgeries aid weight loss, dietary and lifestyle modifications remain essential:
-
Post-Surgery Diet:
-
Clear liquids initially, gradually progressing to soft and solid foods
-
High-protein intake for muscle preservation
-
Small, frequent meals to prevent discomfort
-
-
Hydration:
-
Sip water throughout the day
-
Avoid drinking during meals to prevent overfilling the stomach
-
-
Supplementation:
-
Multivitamins, iron, B12, calcium, and vitamin D as prescribed
-
-
Exercise:
-
Begin with light activity after recovery
-
Progress to aerobic and resistance training for long-term weight management
-
Benefits of Weight Loss Surgery
-
Rapid and sustainable fat loss
-
Improved metabolic health (blood sugar, cholesterol, blood pressure)
-
Enhanced mobility and physical activity tolerance
-
Psychological improvements: Better mood and self-esteem
These outcomes often translate into a reduction in obesity-related morbidity and mortality, reinforcing the value of bariatric interventions when combined with lifestyle changes.
Precautions and Best Practices
-
Surgery is not a quick fix; commitment to diet, exercise, and follow-up care is mandatory.
-
Nutrient deficiencies are common—lifelong supplementation may be required.
-
Psychological support helps manage behavioral changes and prevent weight regain.
-
Select experienced surgeons and accredited centers for optimal outcomes.
FAQs About 5 Weight Loss Surgery Options
1. Which weight loss surgery is most effective?
BPD/DS often results in the highest and fastest weight loss but carries greater nutritional risk.
2. Which surgery is safest?
Sleeve gastrectomy is commonly considered the safest option with lower complication rates.
3. Can I regain weight after surgery?
Yes, without adherence to diet, exercise, and follow-up care, weight regain is possible.
4. How long is recovery?
Hospital stay ranges from 1–5 days, with full recovery over 4–6 weeks depending on the procedure.
5. Are there non-surgical alternatives?
Endoscopic procedures like ESG or medically supervised weight loss programs may be options for less severe cases.
6. Will surgery resolve obesity-related diseases?
Many patients experience remission of diabetes, hypertension, and sleep apnea, but individual results vary.
5 Weight Loss Surgery Options Conclusion
The 5 weight loss surgery options—gastric bypass, sleeve gastrectomy, adjustable gastric band, BPD/DS, and endoscopic sleeve gastroplasty—offer diverse approaches to achieve significant fat loss and improve overall health. Each option has distinct benefits, risks, and suitability profiles. Choosing the right procedure requires consultation with qualified medical professionals, evaluation of health status, and commitment to long-term lifestyle changes. When done correctly, bariatric surgery can transform lives, enhancing both physical and psychological well-being.